Osteoarthritis is a condition that affects the articular cartilage. The articular cartilage is the outer coating at the end of bones.
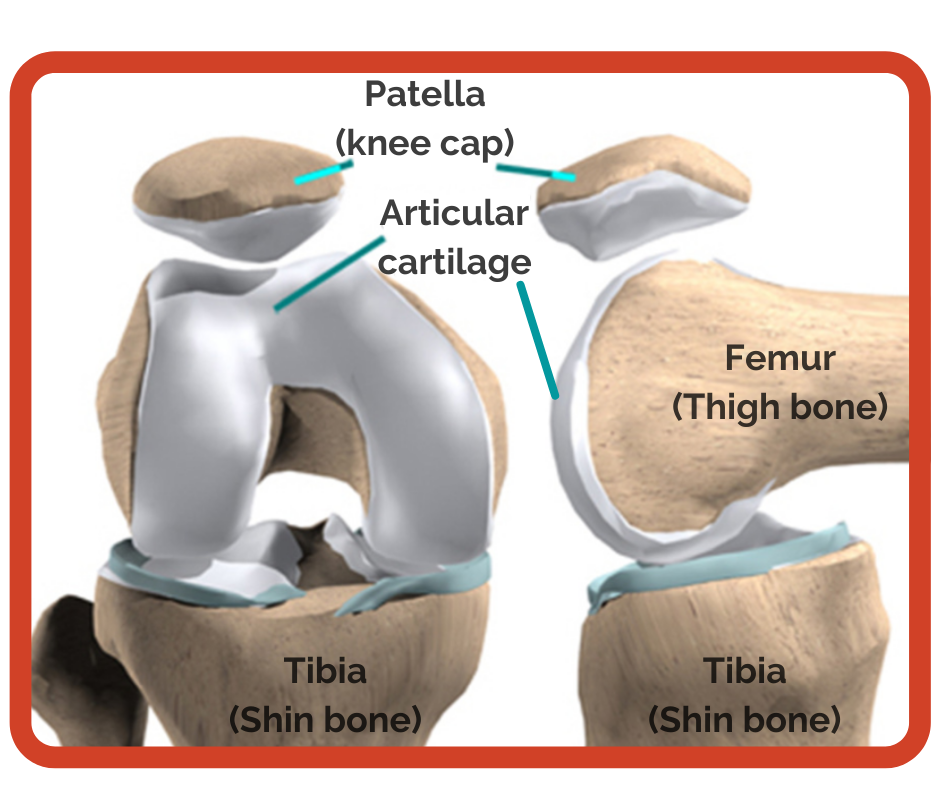
In osteoarthritis, the articular cartilage becomes thin and fragile. This can be due to:
- Healthy cartilage being exposed to heavy loads over a long period of time OR
- Unhealthy cartilage that for some reason cannot handle normal loads.
You may have heard osteoarthritis described as ‘wear and tear’ of the joint leaving ‘bone on bone’. This statement is incorrect, new research has helped us to understand that osteoarthritis pain is most likely caused by a joint working extra hard to repair itself. This causes cartilage to thin, crack, and maybe disappear. However, cartilage needs a certain amount of load to regenerate. This is why healthy loads need to be applied on joints for cartilage recovery. It is important to know that even if the cartilage is thin or damaged there will always be space between the bones.
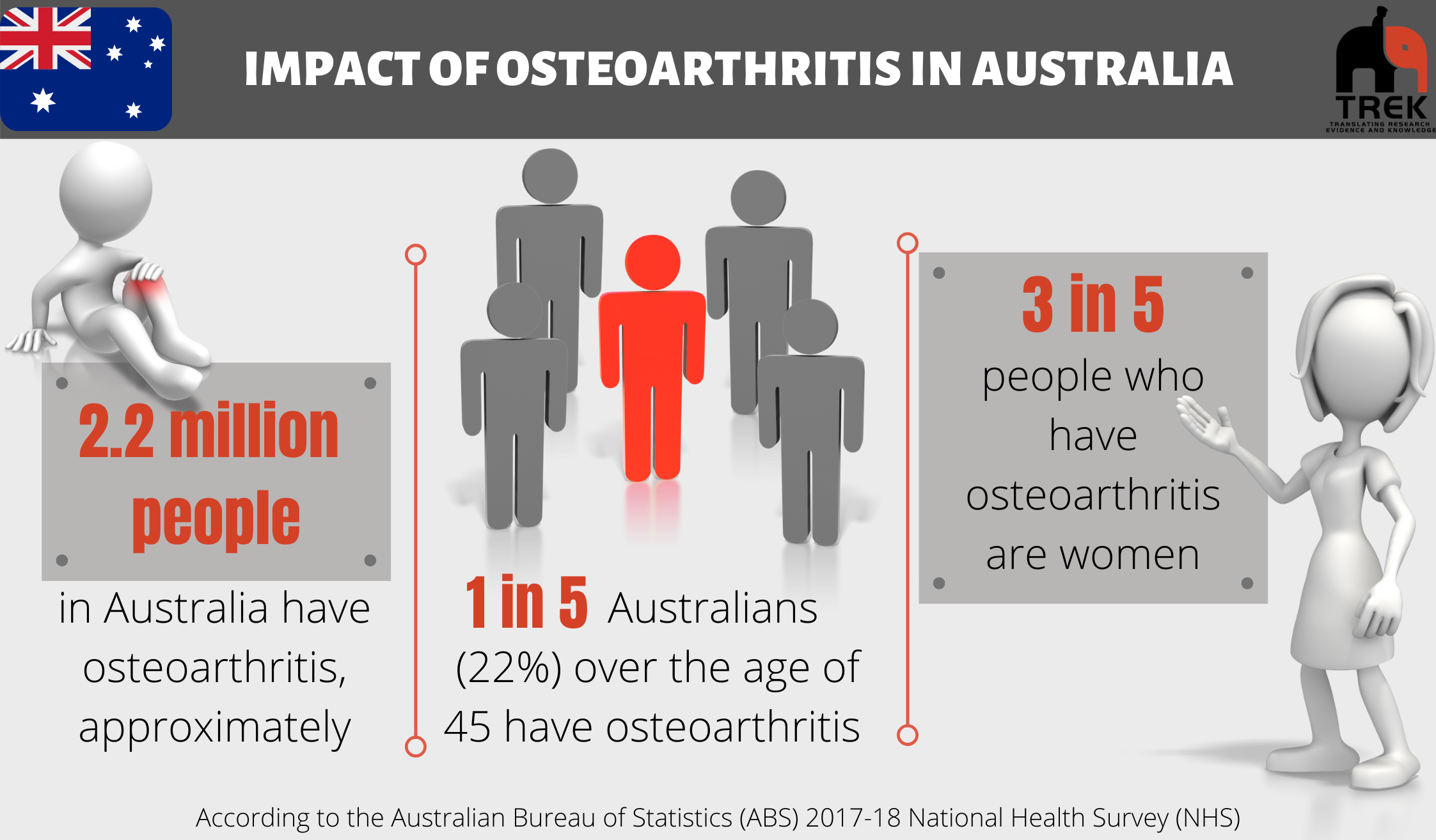
Osteoarthritis can affect any joint but occurs most often in the knees, hips, finger joints and big toe. The knee joints are often affected due to the loading that these joints undergo on a regular basis.
Many people think that an X-ray is essential for diagnosing knee osteoarthritis – but clinically, it is common to diagnose based on symptoms alone.
See the information below to find out more about the symptoms used to diagnose osteoarthritis, and what can show up on imaging: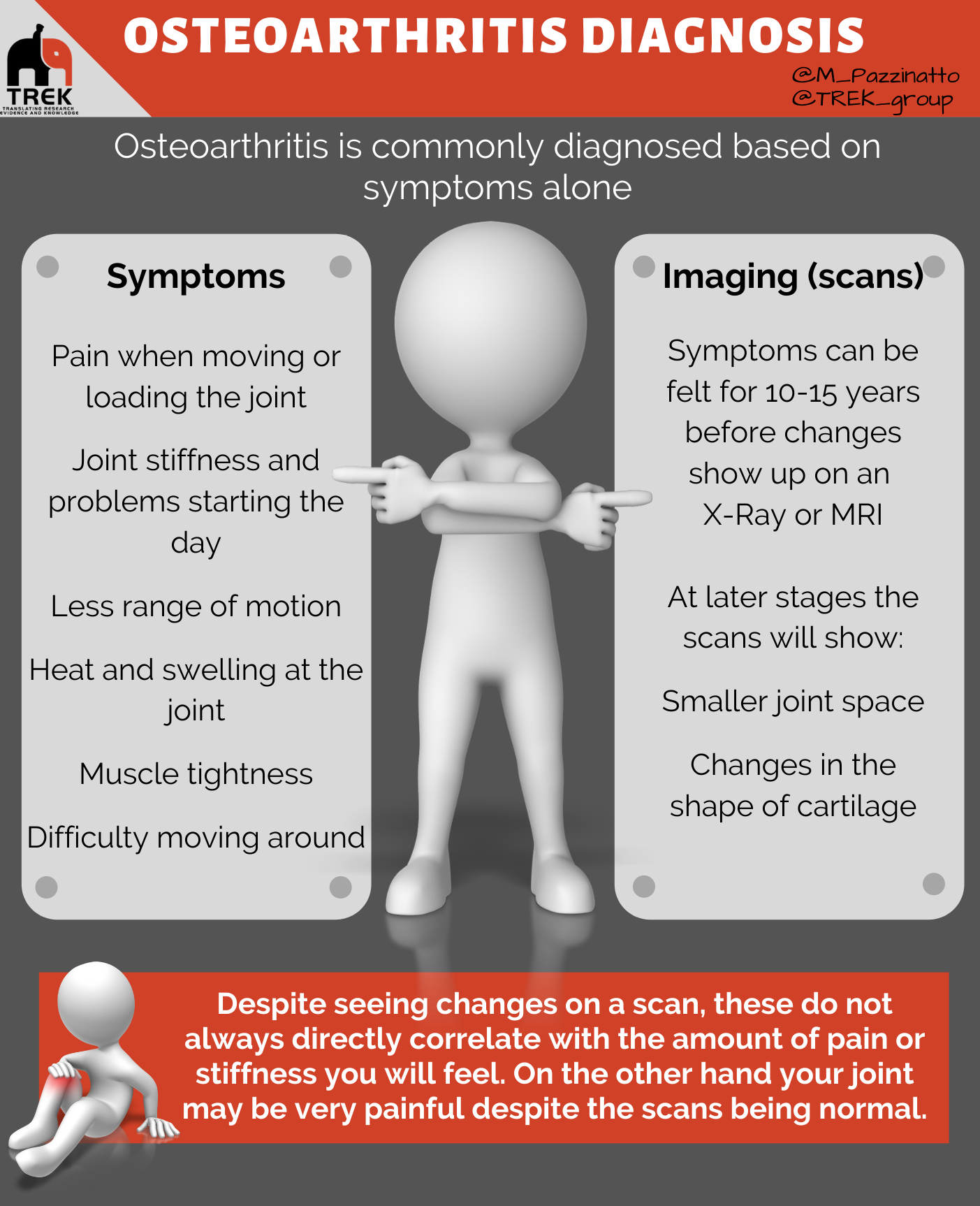
Symptoms
Osteoarthritis often affects one joint and symptoms normally progress slowly. Symptoms can start for no apparent reason. For some people, symptoms stop fully. For others, symptoms quickly turn into more serious problems and spread to other joints. Symptoms can come and go. Early symptoms are more commonly felt in the morning for long periods of time. These include:
- Pain when moving or loading the joint. In time, pain can happen at rest or at night.
- Joint stiffness and problems starting your day.
- Less range of motion.
- Heat and swelling at the joint.
- Muscle tightness.
- Difficulty moving around.
At this time, we can’t predict how each person will experience osteoarthritis.
Imaging (scans)
X-Ray or MRI
Symptoms can be felt for 10-15 years before changes show up on an x-ray or Magnetic Resonance Imaging (MRI). This is why diagnosis for osteoarthritis is done based on symptoms described above.
At later stages, osteoarthritis can be seen on an x-ray or MRI. It will show a smaller joint space and changes in the shape of your jointer the cartilage. However x-rays or MRIs do not diagnose how much trouble you will have. It is important to note that despite seeing changes on a scan, these do not always directly correlate with the amount of pain or stiffness you will feel. On the other hand your joint may be very painful despite the scans being normal.
Osteoarthritis is a very common condition.
There is not one simple reason why you may have osteoarthritis – it is more likely a combination of non-modifiable and modifiable factors.
Non-modifiable factors
(things that raise your chance of getting osteoarthritis that we cannot affect)

Age
Cartilage is a living tissue that can age and weaken over the years. Osteoarthritis can happen at the early age of 30. However, people are more likely to have osteoarthritis after the age of 50.
Sex
Women get osteoarthritis more often than men. Women get osteoarthritis more often in the knees and hands. Men get osteoarthritis more often in the hips.
Hereditary
Delicate cartilage can run in the family. So, you are more likely to get osteoarthritis if someone in your family had it too.
Modifiable factors
(things that can be modified to reduce the risk or reduce the severity of osteoarthritis)
Obesity
Being overweight puts more load on the joint. This can increase the risk of osteoarthritis in the knee. The risk of hand and hip osteoarthritis also increases with obesity. This tells us that other things about being overweight can be linked to getting osteoarthritis.
Physical Inactivity
Little or no load on cartilage is not enough for regeneration. This happens when someone is not active enough. Cartilage needs a healthy amount of load to regenerate.
Muscle weakness
Weak muscles won’t provide proper support to a joint. This leads to more loads being applied to areas of cartilage that don’t take weight well. This can overload the cartilage and increase the risk for knee osteoarthritis.
Role of previous injuries
Sports related joint injury
Half of all people with a severe knee injury (meniscus or cruciate ligament injury), often from sports, get osteoarthritis 10-15 years later. Most people hurt their knee as a teenager, which means that they can get osteoarthritis in their 30s. Top level sports can cause great loads on the whole body without allowing for regeneration. This can lead to degeneration of cartilage.
Work or leisure time related joint injury
Lots of load over a long period of time without rest can cause osteoarthritis later in life. People who work as labourers (farmers, firefighters, etc.) are more at risk of hip and knee osteoarthritis. Teachers seem to get more hand osteoarthritis.
